
Highlights importance of History
Coronary artery disease is often perceived as a problem of middle-aged or elderly patients. However, this case is a powerful reminder that significant atherosclerotic coronary disease can be present even in a very young individual, particularly when risk factors such as familial hyperlipidemia, hypertension, and strong family history of premature coronary artery disease are present.
This case of a 36-year-old male business professional demonstrates several important lessons in modern cardiology. First, typical anginal symptoms should never be ignored, even if initial non-invasive testing appears reassuring. Second, a negative treadmill test does not always exclude severe ischemic heart disease, particularly in the presence of multivessel disease or balanced ischemia. Third, careful clinical assessment and timely coronary angiography can be life-saving in such patients.
This was a young male with familial HLP, classic exertional angina, a reportedly negative TMT, and eventually proven severe critical triple vessel disease, which was managed with multivessel percutaneous coronary intervention (MVPCI).
Clinical Background
The patient was a 36-year-old male, a business professional, non-diabetic, with recently detected hypertension. Despite his young age, his symptom profile was highly suspicious for obstructive coronary artery disease. He had been experiencing typical angina for nearly three months, with pain radiating to the left arm, hand, and fingers, strongly suggesting myocardial ischemia.
His risk profile was especially concerning. There was a positive family history of premature coronary artery disease associated with familial hyperlipidemia, with his father reportedly having severe triple vessel disease treated with CABG approximately 15 years earlier. On laboratory assessment, the patient had markedly elevated total cholesterol and LDL cholesterol, supporting a strong lipid-driven atherosclerotic tendency.
Although his ECG and echocardiogram were normal, and a treadmill test performed elsewhere was reported as negative for ischemia, the patient continued to have clinically significant angina. Importantly, the family recognized the similarity of this presentation to the father’s earlier disease, which prompted consultation for further cardiology evaluation.
History
The most important part of this case is the history. In young patients, physicians may sometimes be falsely reassured by age alone, especially when initial investigations are normal. But in this case, the symptom pattern was classic.
Key historical features included:
-
Young age, but not low risk
-
Recently diagnosed hypertension
-
Elevated total cholesterol and LDL cholesterol
-
Strong family history of premature CAD with familial lipid abnormality
-
Ongoing typical exertional angina
-
Pain radiating to the left upper limb and fingers
-
Persistent symptoms over three months despite prior evaluation
This combination made the pre-test probability of coronary artery disease high, regardless of the negative TMT result.
Why the Negative TMT Did Not Exclude Serious CAD
A treadmill test is a useful screening tool, but it is not infallible. A negative result does not completely rule out ischemic heart disease, especially in select clinical settings.
In this patient, there are several possible explanations for a false negative TMT:
-
Balanced ischemia in severe multivessel coronary artery disease can reduce the relative ECG changes usually used to detect ischemia.
-
The test may not have captured the full severity of symptoms or hemodynamic response.
-
Clinical angina during stress may have been underappreciated if ECG criteria alone were emphasized.
-
Young patients with high functional reserve may sometimes complete exercise with delayed or subtle objective changes.
In this case, the presence of exertional angina during stress despite a negative TMT report should have immediately raised concern. Clinical history outweighed the test interpretation.
TMT Report
The treadmill test, as documented, was reported negative for inducible ischemia because of the absence of significant ST depression. However, the clinical context tells a different story. A patient with a strong family history, marked dyslipidemia, new hypertension, and classic exertional angina cannot be safely categorized as low risk merely because ST changes were absent.
This is one of the most important educational points from this case: a test result must always be interpreted in the context of symptoms and pre-test probability.

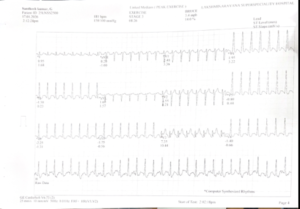
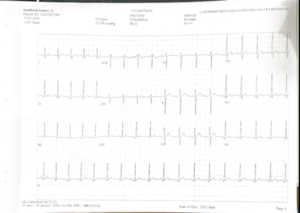
TMT Baseline & Peak exercise tracings
The baseline and peak exercise tracings are important because they allow closer evaluation of the electrical response during exercise. Even when classic diagnostic ST depression is not obvious, the overall exercise response must be assessed together with symptoms, heart rate behavior, blood pressure changes, and exercise-induced chest pain.
In this patient, the exercise tracing becomes especially relevant because the absence of dramatic ECG changes did not match the severity of the patient’s symptoms. This mismatch between clinical presentation and investigation report should always trigger further work-up in a patient with a high-risk profile.
Decision for Coronary Angiography
Because of the classic nature of angina and the strength of the family history, invasive coronary angiography was justified despite the prior non-invasive result. This step proved decisive.
Coronary angiography remains the gold standard for defining coronary anatomy in patients with persistent angina and high suspicion of obstructive disease. In this case, it revealed what the treadmill test failed to show clearly: severe critical triple vessel coronary artery disease.
This finding dramatically changed the management pathway from reassurance to urgent revascularization strategy.
Baseline Coronary Angiogram – LAD
The angiographic assessment of the left anterior descending artery demonstrated significant critical disease. In a young patient, severe LAD disease is especially important because of the large myocardial territory supplied by this vessel. Obstruction in the LAD carries major implications for ischemia, infarction risk, and long-term prognosis.
The angiogram confirmed that this patient’s symptoms were not functional, anxiety-related, or non-cardiac. They were due to genuine flow-limiting coronary lesions.
Baseline Coronary Angiogram – LAD
Baseline Coronary Angiogram – LAD & OM
The angiographic images of the LAD and obtuse marginal territory further established the extent of disease. Multivessel involvement in such a young patient strongly supports an aggressive atherosclerotic process, likely accelerated by inherited lipid abnormality and family predisposition.
Disease affecting both anterior and lateral wall supply territories explains why symptoms were significant despite the misleading treadmill result. It also reinforces the possibility that diffuse ischemic burden may have reduced the sensitivity of the non-invasive test.
Baseline Coronary Angiogram – LAD & OM
Baseline Coronary Angiogram – Lcx & RCA
The angiographic demonstration of disease in the left circumflex and right coronary artery completed the picture of triple vessel disease. At this point, the case clearly represented severe diffuse coronary pathology rather than single-vessel focal disease.
This is a major teaching point: young age does not protect against extensive coronary disease when familial and metabolic risk factors are strong.
The combination of LAD, LCX/OM, and RCA disease also explains why the patient’s ischemic burden may have been underestimated by treadmill ECG criteria alone.
Baseline Coronary Angiogram – Lcx & RCA
Revascularization Strategy and MVPCI
Once severe triple vessel disease was identified, the need for revascularization was clear. In this case, the patient underwent multivessel PCI (MVPCI). Such an approach requires careful lesion assessment, guidewire passage, lesion preparation, stent deployment, and optimization across multiple target vessels.
Because the patient was young and symptomatic, restoring coronary perfusion efficiently was critical not only for relief of symptoms but also for long-term myocardial protection.
LAD – PTCA /LAD wire & Post Predilatation
The initial interventional step in the LAD involved guidewire placement and lesion preparation with balloon dilatation. Predilatation is often necessary in significant calcified or tight stenotic lesions to create an adequate lumen for stent delivery and expansion.
This stage is technically important because proper lesion preparation influences final stent expansion, apposition, and long-term patency.
LAD – PTCA /LAD wire & Post Predilatation
LAD Stent Placement
Following successful wiring and lesion preparation, stent placement in the LAD was performed. Given the critical importance of the LAD, accurate positioning and full expansion were essential.
Stenting of the LAD in a young patient with high atherosclerotic burden is not just a technical act but a major prognostic intervention. A well-executed LAD PCI can significantly reduce ischemic symptoms and prevent major cardiac events.
LAD Stent Placement
Post LAD stent – diag. occlusion
Following LAD stenting, the patient developed chest pain with ECG changes due to diagonal branch occlusion. This is a recognized procedural complication, especially when treating bifurcation-related lesions or lesions near important side branches.
This event highlights the need for constant procedural vigilance. Side branch compromise can convert a technically successful main vessel stent deployment into an incomplete functional result if the occluded branch supplies clinically relevant myocardium.
In this young patient, the diagonal occlusion was not trivial and could not be ignored. The recurrence of chest pain and ECG changes meant the side branch needed to be assessed and reopened.
Post LAD stent – diag. occlusion
Post POBA to Diagonal – flow restored/Post Lad POT – final result – good.
After plain old balloon angioplasty to the diagonal branch, flow was restored, and post-LAD proximal optimization technique (POT) produced a good final result. This sequence is crucial in bifurcation intervention because restoring side-branch patency and optimizing stent geometry improves both immediate and long-term outcomes.
The final angiographic appearance after correction of the diagonal occlusion confirmed technical success and good distal flow.
Post POBA to Diagonal – flow restored/Post Lad POT – final result – good.
LCX/OM Pci – Pre & Post Stent
The circumflex/obtuse marginal territory also underwent PCI. The pre- and post-stent comparison demonstrates the severity of baseline disease and the effectiveness of revascularization.
Treating the LCX/OM territory is important in multivessel disease because untreated lateral wall ischemia can continue to produce symptoms and leave substantial myocardium at risk. In a complete MVPCI strategy, every major ischemia-producing lesion must be addressed thoughtfully.
LCX/OM Pci – Pre & Post Stent
RCA – Pre & Post Stent
The right coronary artery lesion was also treated successfully with PCI and stenting. This completed the multivessel revascularization strategy.
Pre- and post-stent imaging in the RCA demonstrates the final stage of comprehensive management in this patient with critical triple vessel disease. Successful RCA intervention, along with LAD and LCX/OM treatment, helped achieve complete coronary revascularization.
RCA – Pre & Post Stent
Why This Case Matters Clinically
This case has strong teaching value for practicing cardiologists, physicians, trainees, and even general practitioners.
1. Typical angina matters more than age
A 36-year-old patient can still have severe obstructive coronary artery disease. Age should never override symptom quality.
2. Family history can be decisive
A history of premature CAD in a first-degree relative, especially in the setting of familial hyperlipidemia, substantially raises risk.
3. Negative TMT does not always mean no CAD
Treadmill testing has limitations. It may be falsely negative in patients with multivessel disease, balanced ischemia, or highly suggestive clinical symptoms.
4. Clinical judgment remains central
No investigation should replace careful history-taking. In this case, history was the key reason coronary angiography was pursued.
5. Young patients may have advanced diffuse atherosclerosis
Marked dyslipidemia and inherited risk can accelerate disease dramatically.
6. MVPCI can be effectively used in selected multivessel disease
With proper planning and technique, multivessel PCI can restore flow in multiple critical territories.
Technical Learning Points from the Intervention
From an interventional cardiology perspective, this case also demonstrates several procedural learning points:
-
Importance of anatomical definition after discordant non-invasive testing
-
Role of staged lesion interpretation in multivessel disease
-
Need for careful LAD lesion preparation before stent deployment
-
Recognition and management of side branch compromise after main vessel stenting
-
Use of POBA and POT in optimizing bifurcation-related outcomes
-
Complete multivessel PCI strategy involving LAD, LCX/OM, and RCA



